Eye Consultation
An eye consultation with Dr Wong typically starts with a review by a qualified and experienced orthoptist.
Orthoptists are experts in diagnosing disorders of eye movement and associated vision problems. The orthoptist will take a detailed history, including questions about your general health and medications. The orthoptist will then test your vision and eye muscles with various tests, as required. Usually, the orthoptist administers eye drops to dilate your pupils for a full ocular examination. The drops may take 20–30 minutes to take effect and their effects may last for a few hours, potentially blurring your vision and increasing light sensitivity. Once your pupils are fully dilated, Dr Wong will then examine you in greater detail – the eye drops facilitate more detailed examination of the internal structures of the eye. Depending on this comprehensive examination, Dr Wong may recommend further specialised testing be performed. Once the examination is complete, Dr Wong will then advise you on a management plan.
Increased light sensitivity can last for up to 6 hours after adminstration of the eye drops. It will help to avoid bright light or wear sunglasses until the drops wear off.
EYE EXAMINATIONS
A ophthalmic eye exam is a comprehensive series of tests conducted by an ophthalmologist to check both your vision and the health of your eyes. Many diseases and conditions can be diagnosed from the eye and since ophthalmologists are also medical specialists, they can identify ocular manifestations of systemic disease, tumours or other anomalies e.g. diabetes, high blood pressure, raised cholesterol levels, brain tumours.
The eye examination may be comprised of many different tests depending on the needs of the patient. Some of the more common tests are listed below.

Ocular Motility
This test determines proper function of the extraocular muscles which move the eyes. The patient is asked to focus on a target with both eyes as it is moved in each of the nine cardinal directions. The examiner assesses the eyes for anomalies, noting the speed, smoothness, range and symmetry of movements and any unsteadiness of fixation.
Refraction or Visual Acuity
This test determines the visual acuity of the eye – sharpness of vision. It is the quantitative measure of the eye’s ability to see an in-focus image at a certain distance – usually 20 feet.
e.g. a person who has 20/20 vision sees objects that are 20 feet away with the same clarity as a person with normal vision, but a person who has 20/40 vision sees at 20 feet only as clearly as a person with perfect vision sees at 40 feet.
Visual Field Testing
The visual field is the entire area of vision that is seen out of each eye, including the corners (peripheral vision). The visual field may be tested as a routine part of an eye examination. The visual field can be affected by numerous disorders of the visual systems – the most common of which is Glaucoma.
A peripheral vision test can be conducted simply by the doctor through gradually moving an object toward the patient’s center of vision from above, below, left, and right. The patient tells the doctor when the moving finger or target is first detected.
Visual fields can be measured more accurately using a Visual Field Analyser. In this test, the patient stares at the center of a large shallow bowl and presses a button whenever a flash of light is detected.
Optical Biometry
This test is performed to to determine the power of the intraocular lens implant for cataract surgery. There are many parameters comprising the calculation: the cornea, the lens, the ocular media, and the axial length of the eye. The IOL Master system accurately measures all of these parameters and uses sophisticated algorithms to then calculate the power of the intraocular lens implant. Despite its complexity, this test is easy to perform and non-invasive.
Dr Wong will discuss the appropriate lens choice with you in the consultation to meet your requirements.
This test has part of its cost rebated my Medicare.
Intraocular Pressure (or Tonometry)
The purpose of this test is to measure the intraocular pressure – pressure within the eye. This type of test is useful in diagnosing types of glaucoma and monitoring their treatment.
Intraocular pressure is measured using a tonometer, which measures the amount of pressure it takes to flatten the cornea. The greater the pressure within the eye, the harder it is to flatten the cornea.
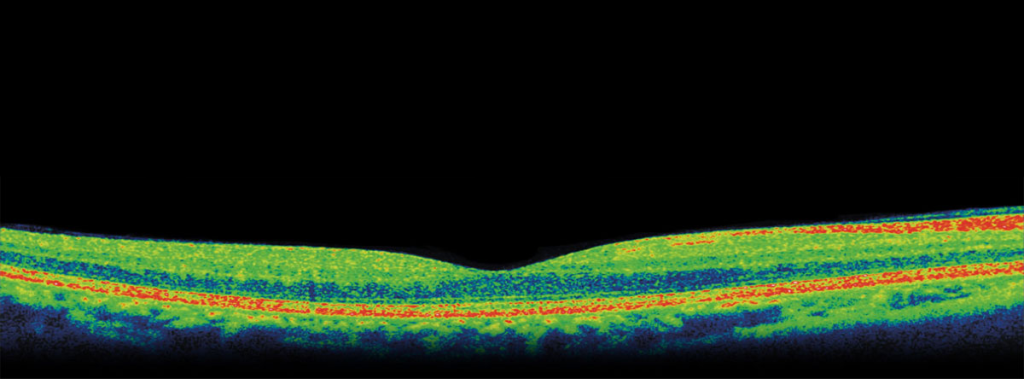
Optical Coherence Tomography (OCT)
Optical Coherence Tomography (OCT) is a non-invasive diagnostic technique using inferometry for producing three-dimensional cross sectional images of the eye. These high resolution images provide a vital tool for the diagnosis and management of anterior (front) and especially posterior (back of the eye) diseases. Images of the retina and optic nerve provide a useful means of monitoring the progress of diseases, such as macular degeneration, diabetes, and glaucoma.
Slit-lamp Examination
A slit lamp is a table mounted binocular microscope with an adjustable light source which allows the doctor to examine the entire eye under high magnification. This exam allows the doctor to see areas at the front of the eye: including the eyelids, conjunctiva, iris, lens, sclera, and cornea..
Eye drops are often used in conjunction with the slit-lamp to dilate the pupils and provide the doctor greater visibility of the back of the eye including the retina and optic nerve as well as the aqueous humor (the fluid in the front part of the eye between the cornea and the iris).
Often, this light source is narrowed to a vertical “slit” – hence the name.